We’re glad you’re taking the opportunity to learn all that you can. Please select a link below for questions relating to that category.
Billing / Business
Medicare Waiver:
According to Centers for Medicare and Medicaid services, the Advance Beneficiary Notice (ABN), is a written notification that must be signed by the patient or guardian prior to the provider rendering a service to a Medicare beneficiary that could potentially be denied/deemed “not medically necessary”. Once a Medicare beneficiary signs the ABN, he or she is legally responsible for the charges if Medicare denies payment for the service.
 Insurance Coverage of Dr.:
Insurance Coverage of Dr.:
Our physicians are contracted with hundreds of different insurance carriers and policies. The best way to verify if your doctor is considered an “in-network” provider is to call your insurance company directly and speak with a patient service representative. At that time, a patient can verify the physicians association with their plan and it would be an ideal time for the patient to ask questions regarding his/her individual policy.
Secondary Insurance Coverage:
The Center for Women will not submit a claim to a secondary insurance unless it is a government funded policy like Medicare, Medicaid, or Tricare. If a secondary insurance is in effect through another carrier, the patient must submit to that carrier on his/her behalf. The front desk staff or the billing office will be more than happy to assist the patient and supply any additional information needed to file.
“Deductible” or “Coinsurance”:
A deductible refers to an annual amount of out-of-pocket expense(s) the subscriber must pay individually and/or per family before benefits are paid by the payer. Coinsurance is the amount of a medical bill for which the beneficiary and/or secondary insurance is fiscally responsible. This amount is represented by a percentage of the billed charges that is specified by the policy plan or, more globally, by the insurance company with whom the beneficiary is affiliated.
Coding and Refiling with my Insurance Company:
It is our policy that all coding discrepancies must be submitted in writing and sent to our financial counselor. The financial counselor will contact the physician directly to review the date of service in question. At that time, the physician will review all medical records, diagnosis codes and procedure codes associated with the visit. The patient will be contacted either by letter or phone to discuss outcome of review.
Insurance Card:
Our front desk representatives will ask to see your current insurance card at each visit. Possessing and presenting your insurance card is the only way to ensure claims are being forwarded to the appropriate payer for processing. For patients that do not have their insurance card at the time of their visit, we do offer other alternatives. Please discuss these options with the representative at the time of your appointment or kindly reschedule your visit.
Contraceptive Methods
The Food and Drug Administration has approved a number of birth control methods, ranging from over-the-counter male and female condoms and vaginal spermicides to doctor-prescribed birth control pills, diaphragms, intrauterine devices (IUDs), injectable hormones, and hormonal implants. Other contraceptive options include fertility awareness and voluntary surgical sterilization. Here are short descriptions of the most popular options:
The Reality Female Condom, approved by FDA in April 1993, consists of a lubricated polyurethane sheath shaped similarly to the male condom. The closed end, which has a flexible ring, is inserted into the vagina, while the open end remains outside, partially covering the labia. The female condom, like the male condom, is available without a prescription and is intended for one-time use. It should not be used together with a male condom because they may slip out of place.
The diaphragm is a dome-shaped rubber disk with a flexible rim that works in two ways to prevent pregnancy. It covers the cervix so sperm can’t reach the uterus, while a spermicide cream or jelly applied to the diaphragm before insertion kills sperm.
The cervical cap is a soft rubber cup with a round rim, sized by a health professional to fit snugly around the cervix. It is available by prescription only and, like the diaphragm, is used with spermicide cream or jelly.
The sponge, a disk-shaped polyurethane device containing the spermicide nonoxynol-9, is not currently marketed but may be sold again in the future. Inserted into the vagina to cover the cervix, the sponge is attached to a woven polyester loop for easier removal.
Vaginal spermicides are available in foam, cream, jelly, film, suppository, or tablet forms. All types contain a sperm-killing chemical. Studies have not produced definitive data on how well spermicides alone prevent pregnancy, but a leading resource for contraceptive information reports the failure rate for typical users may be 26 percent per year.
Typically called “the pill,” combined oral contraceptives have been on the market for over 40 years and are the most popular form of reversible birth control in the United States. This form of birth control suppresses ovulation (the monthly release of an egg from the ovaries) by the combined actions of the hormones estrogen and progestin.
Today’s pills have lower doses of hormones than earlier birth control pills. This has greatly lowered the risk of side effects; however, there are both benefits and risks with taking birth control pills. Benefits include having more regular and lighter periods, fewer menstrual cramps; and a lower risk for ovarian and endometrial cancer, and pelvic inflammatory disease (PID). Serious side effects include an increased chance, for some women, of developing heart disease, high blood pressure, and blood clots. Minor side effects include nausea, headaches, sore breasts, weight gain, irregular bleeding and depression. Many of these side effects go away after taking the pill for a few months. Women who smoke, are over age 35, or have a history of blood clots or breast or endometrial cancer are more at risk for dangerous side effects and may not be able to take the pill. Talk with your doctor or nurse about whether the pill is right for you.
Although taken daily like combined oral contraceptives, minipills contain only the hormone progestin and no estrogen. They work by reducing and thickening cervical mucus to prevent sperm from reaching the egg. They also keep the uterine lining from thickening, which prevents a fertilized egg from implanting in the uterus. These pills are slightly less effective than combined oral contraceptives.
Depo-Provera (depot medroxyprogesterone acetate, or DMPA), approved by FDA in 1992, is injected by a health professional into the buttocks or arm muscle every three months. Depo-Provera prevents pregnancy in three ways: It inhibits ovulation, changes the cervical mucus to help prevent sperm from reaching the egg, and changes the uterine lining to prevent the fertilized egg from implanting in the uterus. The progestin injection is extremely effective in preventing pregnancy, in large part because it requires little effort for the woman to comply: She simply has to get an injection by a doctor once every three months.
Norplant, approved by FDA in 1990, and the newer Norplant 2, approved in 1996, are the third type of progestin-only contraceptive. Made up of matchstick-sized rubber rods, this contraceptive is surgically implanted under the skin of the upper arm, where it steadily releases the contraceptive steroid levonorgestrel. The six-rod Norplant provides protection for up to five years (or until it is removed), while the two-rod Norplant 2 protects for up to three years. Norplant failures are rare, but are higher with increased body weight.
An IUD is a mechanical device inserted into the uterus by a health-care professional. Two types of IUDs are available in the United States: the Paragard CopperT 380A and the Progestasert Progesterone T. The Paragard IUD can remain in place for 10 years, while the Progestasert IUD must be replaced every year. It’s not entirely clear how IUDs prevent pregnancy. They seem to prevent sperm and eggs from meeting by either immobilizing the sperm on their way to the fallopian tubes or changing the uterine lining so the fertilized egg cannot implant in it.
Natural family planning, or the “rhythm method,” depends on not having sexual intercourse or using a barrier method of birth control on the days of a woman’s menstrual cycle when she is more likely to become pregnant. Because a sperm may live in the female’s reproductive tract for up to seven days and the egg may remain fertile for about 24 hours, a woman could get pregnant from intercourse that occurred from seven days before ovulation to 24 hours or more after. Methods to approximate when a woman is fertile are usually based on the menstrual cycle, changes in cervical mucus, or changes in body temperature.
Withdrawal. In this method, also called coitus interruptus, the man withdraws his penis from the vagina before ejaculation. Fertilization is prevented if the sperm don’t enter the vagina. Effectiveness depends on the male’s ability to withdraw before ejaculation. Also, withdrawal doesn’t provide protection from STDs, including HIV. Infectious diseases can be transmitted by direct contact with surface lesions and by pre-ejaculatory fluid.
Female sterilization blocks the fallopian tubes so the egg can’t travel to the uterus. Sterilization is done by various surgical techniques, usually under general anesthesia.
A vasectomy involves sealing, tying or cutting a man’s vas deferens, which otherwise would carry the sperm from the testicle to the penis. Vasectomy involves a quick operation, usually under 30 minutes, with possible minor postsurgical complications, such as bleeding or infection.
A Vaginal Ring is a thin, transparent, flexible ring that you insert into the vagina yourself to provide contraception protection. Leaving the Vaginal Ring in for 3 weeks, it slowly releases estrogen and progestin hormones into the body. These hormones stop ovulation and thicken the cervical mucus, creating a barrier to prevent sperm from fertilizing an egg. Worn continuously for three weeks followed by a week off, each Vaginal Ring provides one month of birth control. The Vaginal Ring is 92-99.7% effective as birth control. It does not protect against sexually transmitted infections, including HIV/AIDS.
ORTHO EVRA® (norelgestromin/ethinyl estradiol transdermal system) known as the birth control patch, delivers a steady flow of hormones through the skin and into your bloodstream over a period of 7 days. ORTHO EVRA contains the same hormones found in the Pill—progestin and estrogen. Some serious health effects have been reported, and the label has been updated to include a new warning and provide additional information on the differences between a weekly transdermal delivery system (the Patch) and a daily oral delivery system (the Pill).
Specifically, the new warning states: “Hormones from patches applied to the skin get into the blood stream and are removed from the body differently than hormones from birth control pills taken by mouth. You will be exposed to about 60% more estrogen if you use ORTHO EVRA than if you use a typical birth control pill containing 35 micrograms of estrogen. In general, increased estrogen exposure may increase the risk of side effects.”
The Essure procedure is a sterilization procedure for women that is performed by an Essure trained doctor. Unlike tubal ligation and vasectomy, there are no incisions. Instead, micro-inserts are passed through the body’s natural pathways (vagina, cervix, and uterus) and placed into your fallopian tubes. During the first 3 months following the procedure, your body and the micro-inserts work together to form a tissue barrier that prevents sperm from reaching the egg. During this period, you will need to use another form of birth control. After 3 months, your doctor will perform a special type of x-ray test called an HSG to confirm that your tubes are completely blocked and you can rely on the Essure micro-inserts for birth control.
Tubal ligation, commonly known as “getting your tubes tied,” is a surgical sterilization technique for women. This procedure closes the fallopian tubes, and stops the egg from traveling to the uterus from the ovary. It also prevents sperm from reaching the fallopian tube to fertilize an egg. In a tubal ligation, fallopian tubes are cut, burned, or blocked with rings, bands or clips. The surgery is effective immediately. Tubal ligations are 99.5% effective as birth control. They do not protect against sexually transmitted infections, including HIV/AIDS.
Two emergency contraceptive pill products have been approved by FDA for use in preventing pregnancy after intercourse when standard contraceptives have failed or when no contraceptives were used at all. One product contains the hormones progestin and estrogen; the other contains just progestin.
Available by prescription or over the counter, both products are believed to work by delaying or inhibiting ovulation, or by keeping a fertilized egg from implanting in the uterine wall. These pills are not effective once the fertilized egg has implanted.
Disclaimer:
Some people wrongly believe that if they take birth control pills, they are protecting themselves not only from getting pregnant but also from infection with HIV and other sexually transmitted diseases (STDs). Birth control pills or other types of birth control, such as intrauterine devices (IUDs), Depo-Provera, or tubal ligation will NOT protect you from HIV and other STDs.
The male latex condom is the only birth control method that is proven to help protect you from HIV and other STDs. If you are allergic to latex, there are condoms made of polyurethane that you can use. Condoms come lubricated (which can make sexual intercourse more comfortable and pleasurable) and non-lubricated (which can be used for oral sex).
Additional Resources & Related Links:
Mammograms
Definition:
A mammogram is a test that is done to look for any abnormalities, or problems, with a woman’s breasts. The test uses a special x-ray machine to take pictures of both breasts. The results are recorded on film that your doctor can examine.
 Mammograms look for breast lumps and changes in breast tissue that may develop into problems over time. They can find small lumps or growths that a doctor or woman can’t feel when doing a physical breast exam. Breast lumps or growths can be benign (not cancer) or malignant (cancer). If a lump is found, a doctor will order a biopsy, a test where a small amount of tissue is taken from the lump and area around the lump. The tissue is sent to a lab to look for cancer or changes that may mean cancer is likely to develop. Finding breast cancer early means that a woman has a better chance of surviving the disease. There are also more choices for treatment when breast cancer is found early.
Mammograms look for breast lumps and changes in breast tissue that may develop into problems over time. They can find small lumps or growths that a doctor or woman can’t feel when doing a physical breast exam. Breast lumps or growths can be benign (not cancer) or malignant (cancer). If a lump is found, a doctor will order a biopsy, a test where a small amount of tissue is taken from the lump and area around the lump. The tissue is sent to a lab to look for cancer or changes that may mean cancer is likely to develop. Finding breast cancer early means that a woman has a better chance of surviving the disease. There are also more choices for treatment when breast cancer is found early.
Types:
There are two reasons mammograms are taken. Screening mammograms are done for women who have no symptoms of breast cancer. Diagnostic mammograms are done when a woman has symptoms of breast cancer or a breast lump. Diagnostic mammograms take longer than screening mammograms because more pictures of the breast are taken.
In January 2000, the FDA approved a new way of doing mammograms, called digital mammography. This technique records x-ray images on a computer, rather than film. It can reduce exposure to radiation, allow the person taking the x-ray to make adjustments without having to take another mammogram, and takes pictures of the entire breast even if the denseness of the breast tissue varies.
Safety:
A mammogram is a safe, low-dose x-ray of the breast. A high-quality mammogram, along with clinical breast exam (exam done by a professional doctor) are the most effective tools for detecting breast cancer early.
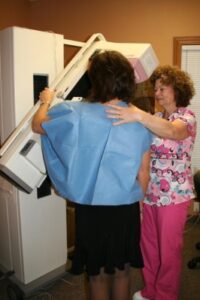
Procedure:
You stand in front of a special x-ray machine. The person who takes the x-rays (always a woman) places your breasts (one at a time) between two plastic plates. The plates press your breast and make it flat. You will feel pressure on your breast for a few seconds. It may cause you some discomfort, feeling like squeezing or pinching. But, the flatter your breasts, the better the picture. Most often, two pictures are taken of each breast – one from the side and one from above. The whole thing takes only a few minutes.
If you have breast implants, be sure to tell your mammography facility that you have them. You will need an x-ray technician who is trained in x-raying patients with implants. This is important because breast implants can hide some breast tissue, which could make if difficult for the radiologist to see breast cancer when looking at your mammograms. For this reason, to take a mammogram of a breast with an implant, the x-ray technician might gently lift the breast tissue slightly away from the implant.
Frequency in Testing:
Women over 40 should get a mammogram every 1 to 2 years. Women who have had breast cancer or breast problems, or with a family history of breast cancer may need to start having mammograms at a younger age or more often. Talk to your doctor about how often you should get a mammogram. Be aware that mammograms don’t take the place of getting breast exams from a doctor and examining your own breasts.
If you find a lump or see changes in your breast, talk to your doctor right away no matter what your age. Your doctor may order a mammogram for you to get a better look at your breast changes.
Limitations of Mammograms:
As with any medical test, mammograms can have limits. These limits include:
- Mammograms are only part of a complete breast exam. If they show abnormalities your doctor will follow-up with other tests.
- False negatives can happen. This means everything may look normal, but cancer is actually present. False negatives don’t happen often. Younger women are more likely to have a false negative mammogram than are older women. This is because the breast tissue is denser, making cancer harder to spot.
- False positives can happen. This is when the mammogram results look like cancer is present, even though it is not. False positives are more common in younger women than older women.
Additional Resources & Related Links:
National “Get A Mammogram: Do It For Yourself, Do It For Your Family” Campaign
(brochures in English, Chinese, Tagalog, and Vietnamese)
National Cancer Institute (NCI)
Phone Number(s): (800) 4-CANCER [800-422-6237]
Internet Address: http://breasthealth.cancer.gov
Menopause
You will feel better by learning all you can about menopause and talking with your doctor about your health and your symptoms. If your symptoms are causing you discomfort or concern, your doctor can teach you about treatment options and help you to make wise treatment choices.
Definition:
Menopause is the time in a woman’s life when her period stops. It is a normal change in a woman’s body. A woman has reached menopause when she has not had a period for 12 months in a row (and there are no other causes, such as pregnancy or illness, for this change). Leading up to menopause, a woman’s body slowly makes less and less of the hormones estrogen and progesterone. This change often happens between the ages of 45 and 55 years old.
Symptoms:
Menopause affects every woman differently. Your only symptom may be your period stopping. You may have other symptoms, too. Many symptoms at this time of life are because of you getting older. But some are due to menopause. Common symptoms of menopause include:
- Change in pattern of periods (can be shorter or longer, lighter or heavier, more or less time between periods)
- Hot flashes (sometimes called hot flushes), night sweats (sometimes followed by a chill)
- Trouble sleeping through the night (with or without night sweats)
- Vaginal dryness
- Mood swings, feeling crabby, crying spells (probably because of lack of sleep)
- Trouble focusing, feeling mixed-up or confused
- Hair loss or thinning on your head, more hair growth on your face
Bone Loss in Menopause:
When a woman is young, estrogen helps to keep bone strong. When estrogen levels fall at menopause, bones weaken. When bones weaken a lot, the condition is called osteoporosis. Weak bones can break more easily.
Managing Menopause:
Eating a healthy diet and exercising at menopause and beyond are important to feeling your best. Most women do not need any special treatment for menopause. But some women may have menopause symptoms that need treatment. Several treatments are available. It’s a good idea to talk about the treatments with your doctor so you can choose what’s best for you. There is no one treatment that is good for all women. Sometimes menopause symptoms go away over time without treatment, but there’s no way to know when.
Hormone Therapy (HT):
If used properly, hormone therapy (once called hormone replacement therapy or HRT) is one way to deal with the more difficult symptoms of menopause. It’s the only therapy that is approved by the government for treating more difficult hot flashes and vaginal dryness. There are many kinds of hormone therapies so your doctor can suggest what’s best for you. As with all treatments, HT has both possible benefits and possible risks; it is important to talk about these issues with your doctor. If you decide to use HT, use the lowest dose that helps and for the shortest time needed. Check with your doctor every 6 months to see if you still need HT. For more information on the benefits and risks of HT, go to http://www.nhlbi.nih.gov/health/women.
Natural Treatments:
Some women decide to take herbal or other plant-based products to help relieve hot flashes. Some of the most common ones are soy and other sources of phytoestrogens. These medications have not been tested by the FDA for safety, drug interactions or efficacy.
Physical Activity:
A woman should first talk to her doctor to see what’s best for her. The goal is to exercise regularly so you can lower the risk of serious disease (such as heart disease or diabetes), and maintain a healthy weight. This usually takes at least 30 minutes of exercise (such as brisk walking) on most days of the week.
Premature Menopause:
Menopause is called “premature” if it happens at or before the age of 40— whether it is natural or brought on by medical means (induced). Having premature menopause puts a woman at more risk for osteoporosis later in her life. For women who want to have children, premature menopause can be a source of great distress. Women who still want to become pregnant can talk with their doctors about other ways of having children, such as donor egg programs or adoption.
Postmenopause:
Postmenopause is the term for all the years beyond menopause. It begins after you have not had a period for 12 months in a row — whether your menopause was natural or medically induced.
Additional Resources & Related Links:
Food and Drug Administration (FDA)
Phone: (888) 463-6332
Internet Address: www.fda.gov/womens/menopause
The North American Menopause Society (NAMS)
Phone: (800) 774-5342
Internet Address: http://www.menopause.org
PMS (Premenstrual Syndrome)
Definition:
Premenstrual syndrome (PMS) is a group of symptoms related to the menstrual cycle. PMS symptoms occur in the week or two weeks before your period (menstruation or monthly bleeding). The symptoms usually go away after your period starts. PMS may interfere with your normal activities at home, school, or work. Menopause, when monthly periods stop, brings an end to PMS.
The causes of PMS are not yet clear. Some women may be more sensitive than others to changing hormone levels during the menstrual cycle. Stress does not seem to cause PMS, but may make it worse. PMS can affect menstruating women of any age.
PMS often includes both physical and emotional symptoms. Diagnosis of PMS is usually based on your symptoms, when they occur, and how much they affect your life.
Symptoms:
PMS often includes both physical and emotional symptoms. Common symptoms are:
- Breast swelling and tenderness
- Fatigue and trouble sleeping
- Upset stomach, bloating, constipation or diarrhea
- Headache
- Appetite changes or food cravings
- Joint or muscle pain
- Tension, irritability, mood swings, or crying spells
- Anxiety or depression
- Trouble concentrating or remembering
Symptoms vary from one woman to another. If you think you have PMS, try keeping track of your symptoms for several menstrual cycles. You can use a calendar to note which symptoms you are having on which days of your cycle, and how bad the symptoms are. If you seek medical care for your PMS, having this kind of record is helpful.
Estimates of the percentage of women affected by PMS vary widely. According to the American College of Obstetricians and Gynecologists, up to 40 percent of menstruating women report some symptoms of PMS. Most of these women have symptoms that are fairly mild and do not need treatment. Some women (perhaps five to ten percent of menstruating women) have a more severe form of PMS.
Treatments:
Many treatments have been tried for easing the symptoms of PMS. However, no treatment has been found that works for everyone. A combination of lifestyle changes and other treatment may be needed. If your PMS is not so bad that you need medical help, a healthier lifestyle may help you feel better and cope with symptoms.
Adopt a healthier way of life. Exercise regularly, get enough sleep, choose healthy foods, don’t smoke, and find ways to manage stress in your life.
Try avoiding excess salt, sugary foods, caffeine, and alcohol, especially when you are having PMS symptoms.
Be sure that you are getting enough vitamins and minerals. Take a multivitamin every day that includes 400 micrograms of folic acid. A calcium supplement with vitamin D can help keep bones strong and may help with PMS symptoms.
In more severe cases, drugs such as diuretics, ibuprofen, birth control pills, or antidepressants may be used.
Although PMS does not seem to be related to abnormal hormone levels, some women respond to hormonal treatment. For example, one approach has been to use drugs such as birth control pills to stop ovulation from occurring. There is evidence that a brain chemical, serotonin, plays a role in severe forms of PMS. Antidepressants that alter serotonin in the body have been shown to help many women with severe PMS.
Additional Resources & Related Links:
Preconception
You have finally made a decision to take the big step — becoming a parent! You may want to visit your doctor and improve your diet. Get to know your body and your cycle so you can recognize when you are ovulating. Preparing for pregnancy can help make sure things start off on the right foot. A pre-pregnancy health check can help you understand why it is so important to visit your doctor before you begin trying to have a child.
The Internet is also a rich source of information on conceiving. For some tips on improving your chances of conceiving, take a look at www.pregnancy-info.net/trying_intro.html. You can also visit Baby Center — Pregnancy, parenting and family planning resource that you can customize to share local resources.
Additional Resources & Related Links:
Planned Parenthood Federation of America
Phone Number: (800) 230-7526
Internet Address: www.plannedparenthood.org
STD’s (Sexually Transmitted Diseases)
The Basics:
Sexually transmitted diseases (STDs) or sexually transmitted infections (STIs), once called venereal diseases, are among the most common infectious diseases in the United States today. More than 20 STIs have now been identified, and they affect more than 13 million men and women in this country each year. The annual comprehensive cost of STIs in the United States is estimated to be well in excess of $10 billion.
It is important to understand at least five key points about all STDs in this country today:
• STIs affect men and women of all backgrounds and economic levels. They are most prevalent among teenagers and young adults. Nearly two-thirds of all STIs occur in people younger than 25 years of age. The incidence of STIs is rising in part because in the last few decades, young people have become sexually active earlier yet are marrying later. In addition, divorce is more common. The net result is that sexually active people today are more likely to have multiple sex partners during their lives and are potentially at risk for developing STIs.
• Most of the time, STIs cause no symptoms, particularly in women. Symptoms may be confused with those of other diseases not transmitted through sexual contact. Even when an STI causes no symptoms, a person who is infected may pass the disease on to a sex partner. That is why many doctors recommend periodic testing or screening for people who have more than one sex partner.
• Health problems caused by STIs tend to be more severe and frequent for women, in part because the frequency of asymptomatic infection means that many women do not seek care until serious problems develop. Some STIs can spread into the uterus (womb) and fallopian tubes to cause pelvic inflammatory disease (PID), which in turn is a major cause of both infertility and ectopic (tubal) pregnancy. The latter can be fatal. STIs in women also may be associated with cervical cancer. One STI, human papillomavirus infection (HPV), causes genital warts and cervical and other genital cancers (see below for more information).
• STIs can be passed from a mother to her baby before, during, or immediately after birth; some of these infections of the newborn can be cured easily, but others may cause a baby to be permanently disabled or even die.
• When diagnosed and treated early, many STIs can be treated effectively. Some infections have become resistant to drugs and require newer types of antibiotics.
HIV Infection & AIDS:
AIDS (acquired immunodeficiency syndrome) was first reported in the United States in 1981. It is caused by the human immunodeficiency virus (HIV), a virus that destroys the body’s ability to fight off infection. An estimated 900,000 people in the United States are currently infected with HIV. People who have AIDS are very susceptible to many life-threatening diseases, called opportunistic infections, and to certain forms of cancer. Transmission of the virus primarily occurs during sexual activity and by sharing needles used to inject intravenous drugs. If you have any questions about HIV infection or AIDS, you can call the AIDS Hotline confidential toll-free number: 1-800-342-AIDS.
Chlamydial Infection:
This infection is now the most common of all bacterial STIs, with an estimated 4 to 8 million new cases occurring each year. In both men and women, chlamydial infection may cause an abnormal genital discharge and burning with urination. In women, untreated chlamydial infection may lead to pelvic inflammatory disease, one of the most common causes of ectopic pregnancy and infertility in women. Many people with chlamydial infection, however, have few or no symptoms of infection. Once diagnosed with chlamydial infection, a person can be treated with an antibiotic.
Genital Herpes:
Herpes infections are caused by herpes simplex virus (HSV). The major symptoms of herpes infection are painful blisters or open sores in the genital area. These may be preceded by a tingling or burning sensation in the legs, buttocks, or genital region. The herpes sores usually disappear within two to three weeks, but the virus remains in the body for life and the lesions may recur from time to time. Severe or frequently recurrent genital herpes is treated with one of several antiviral drugs that are available by prescription. These drugs help control the symptoms but do not eliminate the herpes virus from the body. Suppressive antiviral therapy can be used to prevent occurrences and perhaps transmission. Women who acquire genital herpes during pregnancy can transmit the virus to their babies. Untreated HSV infection in newborns can result in mental retardation and death.
Genital Warts:
Genital warts (also called venereal warts or condylomata acuminata) are caused by human papillomavirus, a virus related to the virus that causes common skin warts. Genital warts usually first appear as small, hard painless bumps in the vaginal area, on the penis, or around the anus. If untreated, they may grow and develop a fleshy, cauliflower-like appearance. Genital warts infect an estimated 1 million Americans each year. In addition to genital warts, certain high-risk types of HPV cause cervical cancer and other genital cancers. Genital warts are treated with a topical drug (applied to the skin), by freezing, or if they recur, with injections of a type of interferon. If the warts are very large, they can be removed by surgery.
Gonorrhea:
The most common symptoms of gonorrhea are a discharge from the vagina or penis and painful or difficult urination. The most common and serious complications occur in women and, as with chlamydial infection, these complications include PID, ectopic pregnancy, and infertility. Historically, penicillin has been used to treat gonorrhea, but in the last decade, four types of antibiotic resistance have emerged. New antibiotics or combinations of drugs must be used to treat these resistant strains.
Syphilis:
The first symptoms of syphilis may go undetected because they are very mild and disappear spontaneously. The initial symptom is a chancre; it is usually a painless open sore that usually appears on the penis or around or in the vagina. It can also occur near the mouth, anus, or on the hands. If untreated, syphilis may go on to more advanced stages, including a transient rash and, eventually, serious involvement of the heart and central nervous system. The full course of the disease can take years. Penicillin remains the most effective drug to treat people with syphilis.
HPV
The human papillomavirus infection, or HPV, is contracted through common exposure upon changing sexual partners or being with a partner that has partners prior to you. HPV can be passed orally, anally or vaginally. There are over 100 strains of HPV; some may cause mild changes to the cervix but severe changes that can arise over time can lead to cancer with high risk strains of HPV. The Center for Women uses PAPs as screening tools to catch these cervical changes but we also screen for symptoms and examine the cervix once a year upon your annual exam.
Other STD’s:
Other diseases that may be sexually transmitted include trichomoniasis, bacterial vaginosis, cytomegalovirus infections, scabies, and pubic lice.
STD’s in Pregnancy:
STDs in pregnant women are associated with a number of adverse outcomes, including spontaneous abortion and infection in the newborn. Low birth weight and prematurity appear to be associated with STDs, including chlamydial infection and trichomoniasis. Congenital or perinatal infection (infection that occurs around the time of birth) occurs in 30 to 70 percent of infants born to infected mothers, and complications may include pneumonia, eye infections, and permanent neurologic damage.
Prevention:
The best way to prevent STDs is to avoid sexual contact with others. If you decide to be sexually active, there are things that you can do to reduce your risk of developing an STD.
- Have a mutually monogamous sexual relationship with an uninfected partner.
- Correctly and consistently use a male condom.
- Use clean needles if injecting intravenous drugs.
- Prevent and control other STDs to decrease susceptibility to HIV infection and to reduce your infectiousness if you are HIV-infected.
- Delay having sexual relations as long as possible. The younger people are when having sex for the first time, the more susceptible they become to developing an STD.
- The risk of acquiring an STD also increases with the number of partners over a lifetime.
Anyone who is sexually active should:
- Have regular checkups for STIs even in the absence of symptoms, and especially if having sex with a new partner. These tests can be done during a routine visit to the doctor’s office.
- Learn the common symptoms of STIs. Seek medical help immediately if any suspicious symptoms develop, even if they are mild.
- Avoid having sex during menstruation. HIV-infected women are probably more infectious, and HIV-uninfected women are probably more susceptible to becoming infected during that time.
- Avoid anal intercourse, but if practiced, use a male condom.
- Avoid douching because it removes some of the normal protective bacteria in the vagina and increases the risk of getting some STIs.
Anyone diagnosed as having an STI should:
- Be treated to reduce the risk of transmitting an STI to an infant.
- Discuss with a doctor the possible risk of transmission in breast milk and whether commercial formula should be substituted.
- Notify all recent sex partners and urge them to get a checkup.
- Follow the doctor’s orders and complete the full course of medication prescribed. A follow-up test to ensure that the infection has been cured is often an important step in treatment.
- Avoid all sexual activity while being treated for an STI.
Sometimes people are too embarrassed or frightened to ask for help or information. Most STIs are readily treated, and the earlier a person seeks treatment and warns sex partners about the disease, the less likely the disease will do irreparable physical damage, be spread to others or, in the case of a woman, be passed on to a newborn baby.
Additional Resources & Related Links:
AIDS Hotline confidential toll-free number: 1-800-342-AIDS
Centers for Disease Control & Prevention
Public Inquiries/MASO
Mailstop E11
1600 Clifton Road
Atlanta, GA 30333
Phone 1-800-311-3435
Internet Address: www.cdc.gov
Urinary Incontinence
Definition:
When you are not able to hold your urine until you can get to a bathroom, you have what’s called urinary incontinence (also called loss of bladder control). In contrast, bladder control means you urinate only when you want to. Incontinence can often be temporary, and is always caused by an underlying medical condition.
More than 13 million Americans experience loss of bladder control. However, women suffer from incontinence twice as often as men do. Older women have more bladder control problems than younger women do. The loss of bladder control, however, is not something that has to happen as you grow older. It can be treated and often cured, whatever your age. Don’t let any embarrassment about incontinence prevent you from talking to your doctor about your condition. Find out if you have a medical condition that needs treatment.
Effects of Pregnancy, Childbirth and Menopause:
During pregnancy, the added weight and pressure of the unborn baby can weaken pelvic floor muscles, which affects your ability to control your bladder. Sometimes the position of your bladder and urethra can change because of the position of the baby, which can cause problems. Vaginal delivery and an episiotomy (the cut in the muscle that makes it easier for the baby to come out) can weaken bladder control muscles. And, pregnancy and childbirth can cause damage to bladder control nerves.
After delivery, the problem of urinary incontinence often goes away by itself. But if you are still having problems 6 weeks after delivery, talk to your doctor. Bladder control problems don’t always show up right after childbirth. Some women do not commonly have problems with incontinence until they reach their 40s.
Menopause (when your periods stop completely) can cause bladder control problems for some women. During menopause, the amount of the female hormone estrogen in your body starts decreasing. The lack of estrogen causes the bladder control muscles to weaken. Estrogen controls how your body matures, your monthly periods, and body changes during pregnancy and breastfeeding. Estrogen also helps keep the lining of the bladder and urethra plump and healthy.
Talk with your doctor about whether taking estrogen to prevent further bladder control problems is best for you. Tell him or her if you or your family has a history of cancer. If you face a high risk of breast cancer or uterine cancer, your doctor may not prescribe estrogen for you.
Diagnostics:
If you are having a problem with incontinence, the first step is to see your doctor. Gynecologists and obstetricians specialize in the female reproductive tract and childbirth. A urogynecologist focuses on urological problems in women. Family practitioners and internists treat patients for all kinds of complaints. Any of these doctors may be able to help you.
To diagnose the problem, your doctor will first ask you about your symptoms and for a complete medical history. You will also be asked about your bladder habits: how often you empty your bladder, how and when you leak urine, or when you have accidents.
Your provider will then do a physical exam to look for signs of any medical conditions that can cause incontinence, such as tumors that block the urinary tract, impacted stool, and poor reflexes that may be nerve-related.
A test may be done to figure out how much your bladder can hold and how well your bladder muscles function. For this test, you will be asked to drink plenty of fluids and urinate into a measuring pan, after which your provider will measure any urine that remains in the bladder. Your provider may also recommend other tests, including a stress test, urinalysis, blood test, ultrasound, cystoscopy, and urodynamics.
You may be asked to keep a diary for a day or a week in order to record when you empty your bladder. This diary should include the times you urinate and the amounts of urine you produce. To measure your urine, you can use a special pan that fits over the toilet rim and is available at drug stores or surgical supply stores.
Treatments:
There are a number of ways to treat incontinence. Your doctor will work with you to figure out which way(s) is best for you. Don’t give up or be embarrassed! Remember, many women have incontinence and all types of incontinence can be treated, no matter what your age.
Treatments include Pelvic muscle exercises, electrical stimulation, biofeedback, timed voiding or bladder training, weight loss, dietary changes, medication, implants, surgery, catheterization, or dryness aids.
Additional Resources & Related Links:
